Doug's Journal
Mitral Regurgitation, Joined February 23, 2025
Mitral Regurgitation
Joined February 23, 2025
-
 I am from: Ames, Iowa
I am from: Ames, Iowa -
 My surgery date is: February 17, 2025
My surgery date is: February 17, 2025









I’m 6 weeks post-op (Surgery ...Read more
I’m 6 weeks post-op (Surgery Feb 17th) from robotic mitral valve repair at Mayo Clinic Rochester. Dr’s Daly and Arghami were my surgeons and Dr Murphy is my Mayo cardiologist.
I’m 56 y/o with a pretty active life. I’m 20 pounds overweight and I like a beer or three, but otherwise a reasonably healthy lifestyle.
Symptoms: I was out of breath with very little exertion, could hear a “gurgling” murmur w/o a stethoscope, and had some mild steady pain in my left heart area.
My Mayo diagnosis was severe mitral valve regurgitation. My fraction was 65%, and my heart was normal sized. Very short period of symptoms before I got in for diagnosis/repair. I live in Iowa and have Wellmark Blue Cross with the “National” option. That’s how I was able to go to Mayo in MN.
I had a p2 flail and 2 ruptured cordae. I have no history of heart disease, nor family history. My arterial blockage “score” was zero on my contrast CT, and all the other testing showed that my heart and circulatory system is in excellent shape. I have never had any other surgical procedures requiring admission. I’ve had COVID several times and got the first three vaccination shots. No severe COVID symptoms or adverse vaccination reactions. I get flu shots and I believe in vaccines.
The repair was to resection the valve flap, sew in a Medtronic annular ring, and repair the ruptured cordae with Gore-Tex material. I was on the heart-lung machine for ~65 minutes and cross clamped for 43. My surgeons said that it was a very fast repair and it went very well. My murmur was gone immediately.
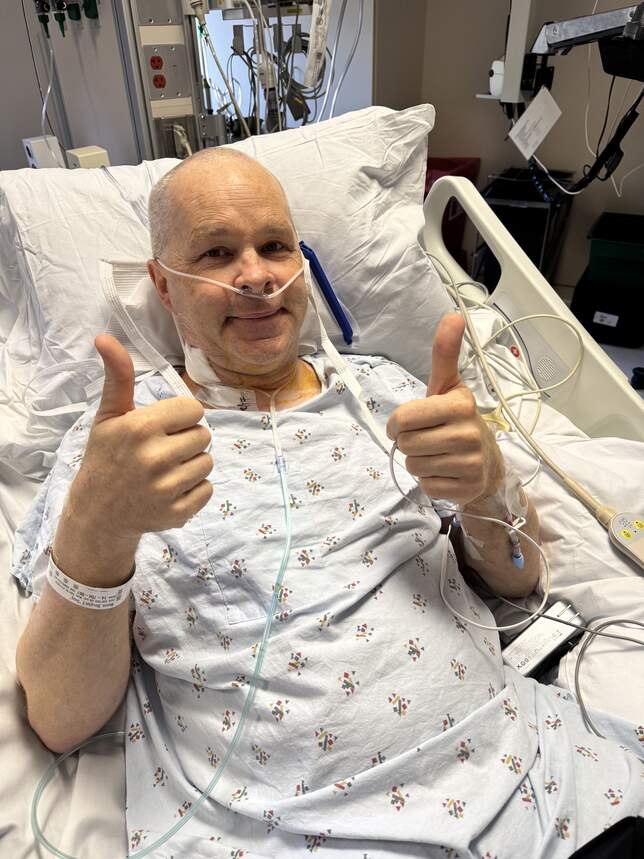
I went into pre-op Monday (Day 0) at 645am. I woke up pretty lucid in the cardiac ICU around 2pm. Photo below was an hour after I woke up. Pain was a 4, predominantly from the chest tubes wiggling around in my chest every time I moved. The catheter was a non issue- didn’t even know it was there, and not having to get up to pee was a real blessing. The femoral and neck lines were still in-I have no idea what those do or if they were attached to something. My breathing tubes were out when I woke up-I'm told this is Mayo’s standard-they come out in the OR. Throat was sore but not more than a bad cold gives you. I could talk freely, but a little scratchy. I stayed in the ICU overnight; constant vital sign checking, water, pills. Not much sleep, but what I did get was decent-drug assisted. My pee bag filled quickly and often.
Tuesday, (Day 1), I moved to the cardiac step-down unit around 11am. Catheter still in, chest tubes still in. Only significant pain was the chest tubes. Pain pills every 4 hours, inc Oxy. Got some food around 2pm, walked a few hundred feet. That night, I was still on monitoring, so regular vital checks etc, but low pain. All my numbers were good and I was peeing a lot. The day is a haze of sleep/wake/vitals/repeat.
Wednesday (Day 2) was a big day: Neck tubes, Femoral tube, Chest tubes came out mid-morning, catheter same. Lot less pain w/o chest tubes. Walked to and used the toilet w/o incident. Bowels not moving, but I was on stool softeners and not uncomfortable. I walked several times Wednesday for increasing lengths. Felt pretty good but definitely was winded and tired afterwards. The day is kind of a blur, except that I ate several small meals, drank a ton of water, had a coffee (good bye caffeine headache), and wrote a bunch of understandable texts and emails to friends and family. That night, they took me off “monitoring” and I was only woken up once for vital signs. Slept well thanks to my earplugs and eye mask. Turned the heat down to what we have at home, 65F.
Thursday (day 3) pain was almost zero, appetite good, I was mobile, and READY TO GO. My bowels cooperated, so that box was checked. All my important numbers must have been good, because there was no delay in sending me home. A discharge nurse came in and went over a bunch of “going home” instructions. We were in the car headed south by 1130am.
I could go on for paragraphs about the level of care at Mayo. I’ll summarize by saying :Mayo is the best hospital in America, maybe the world.
I hope this is helpful. The fear of the unknown was much worse than the reality. I’m happy to answer any questions.